The Video Game the Body Plays Without Knowing It

How MindfulGarden is using biofeedback, nature, and a partnership with PHC Ventures to change how hospitals treat delirium without reaching for a vial.
Imagine a hospital bed in a busy intensive care unit (ICU). A patient, someone’s mother, father, grandparent, suddenly doesn’t know where they are. They’re confused, frightened, agitated. They may pull at their IV lines, call out, or try to get up. The nurse on shift has a dozen other patients. While best practice calls for calm reorientation, mobilization, and human‑centred care, the reality of time pressure and risk can mean patients are instead sedated or restrained, measures meant to protect safety, but which may worsen delirium.
MindfulGarden believes there is a better way. Now, with the support of PHC Ventures and a clinical partnership at St. Paul’s Hospital (SPH), they have the evidence to prove it.

A Preventable Tragedy That Sparked an Idea
MindfulGarden’s story begins not in a lab, but in a hospital room. Mark Ross, co-founder and CTO, recalls the moment that set everything in motion. His co-founder’s mother — a healthy senior — went in for an elective hip replacement at a regional hospital. What happened next was a cascade of failures familiar to far too many families. What happened next was a cascade of failures familiar to far too many families.
“She developed a post-surgical delirium, became highly agitated and aggressive,” Ross explains. “Unfortunately, the delirium wasn’t properly diagnosed. Given her age, they assumed it was someone with dementia. Because she was so aggressive, she was treated with a heavy course of antipsychotics and restraints over an extended period, which ultimately contributed to her passing. It was a terrible and preventable death.”
Out of that tragedy came a wave of determination. First from nurses who said, “we have to do better,” and then from Ross and his team, who had been building large-scale interactive environments for events like the Olympics. A geriatric nurse saw their work and asked a deceptively simple question: could you miniaturize this and bring it bedside for frail elderly patients?
That answer was MindfulGarden.
What Delirium Is — and Why It Matters
Delirium is a sudden, acute disruption of brain function characterized by confusion, agitation, and disorientation. It affects an estimated 70% of critical care patients and 30% of hospital patients overall. Unlike dementia, it can be reversed, but only if it is properly recognized and managed.
The human and economic costs are staggering. Delirium is associated with 3x higher in-hospital mortality, 2.5x greater cost of care, 2.5x increased readmission rates, and a 9x greater risk of future cognitive decline. Across North America, the direct cost to healthcare systems is estimated at $92 billion annually.
$92B
Direct annual cost of delirium to North American healthcare systems
70%
Of critical care patients affected by delirium
25.7%
Reduction in as-needed antipsychotic use in MindfulGarden’s foundational clinical study
9X
Greater risk of future cognitive decline associated with hospital-acquired delirium
In the past, the standard clinical response has been pharmacological: antipsychotics to sedate, restraints to immobilize. But research increasingly documents the devastating short and long-term consequences of this approach — and clinicians are actively searching for alternatives.
“Delirium is one of the areas where we really don’t have effective treatments, so we tend to give drugs. This is a great opportunity to address that gap.”
— Dr. Alana Flexman, Anesthesiologist and Researcher, SPH
A Video Game the Body Plays Without Knowing
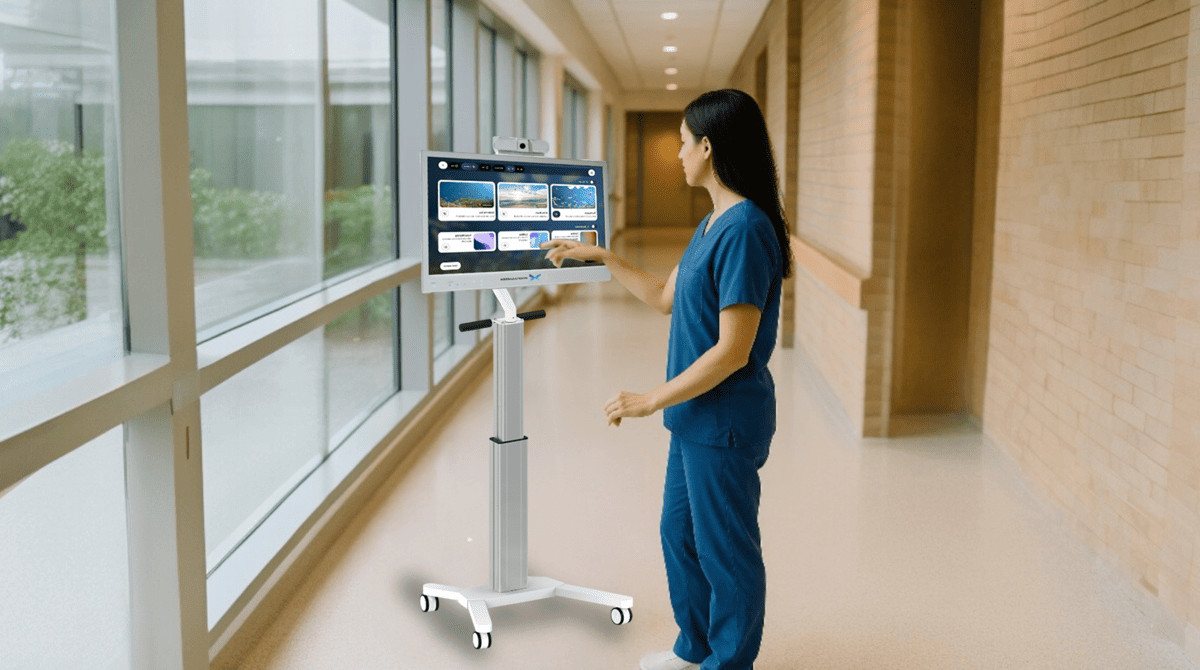
MindfulGarden’s platform is built on a game engine and deployed on a large format touchscreen, the kind of wheeled workstation already familiar in hospital environments. There are no VR headsets, no wearables, nothing that might further agitate a distressed patient.
Through a camera and microphone, the device continuously captures proxies for agitation: vocalizations, movement, and — in the next generation — vital signs. These inputs drive a layered, nature-based audiovisual experience that responds in real time to what the patient’s body is doing. As the patient calms, the visuals shift. The environment mirrors their state and gently guides them toward homeostasis.
“Some nurses call it the video game the patient doesn’t know they’re playing,” says Ross. “I’ve been using that ever since I first heard it. In even simpler terms, it’s distraction therapy but with a closed feedback loop.”
The platform requires no hospital IT integration, collects no personal health information, and can be up and running after minutes of training. It is designed to be the first reach: a calming intervention deployed before medication is even considered, without interrupting clinical workflow.
The Ventures Bridge from Idea to Evidence
For any health technology, clinical validation is the critical threshold between a promising idea and a deployable product. It is also one of the hardest thresholds to cross, requiring clinical champions, institutional trust, research infrastructure, and a path through complex contracting and ethics processes.
This is where PHC Ventures played a pivotal role for MindfulGarden.
The connection began through Creative Destruction Labs’ biomedical engineering stream, where MindfulGarden first encountered PHC Ventures’ leadership. From there, Ventures helped broker a relationship with Dr. Alana Flexman, an anesthesiologist and researcher at SPH whose interests were a near-perfect match for MindfulGarden’s clinical thesis.
“Ventures matched us very well,” says Dr. Flexman. “Delirium is one of my areas of research interest, and their product was very aligned. Sometimes you get approached by other groups and it’s just not your research interest — you’re not going to invest as much time. But this was a very good match of mutual interest.”
Beyond the introduction, PHC Ventures served as the operational backbone that made the evaluation possible. Because of the organizational structure of Providence Health Care (PHC), MindfulGarden could not contract directly with the hospital, PHC Ventures provided the contracting vehicle that allowed all parties to move forward.
“It was really quite smooth and seamless,” says Ross. “When you have a clear picture of what you want to do and what the roles and responsibilities are, it’s easy to move things along. All told, there were maybe two meetings and then back and forth by email over less than a month. In healthcare circles, that’s pretty quick.”
“There is no substitute for talking to clinicians. They are incredibly candid and honest. They will tell you exactly what works and what doesn’t, and when you have assumptions about something that works and it doesn’t, they will tell you. It stops us going down the wrong path.”
— Mark Ross, Co-Founder & CTO, MindfulGarden
What Happened in the Hospital
The PHC Ventures-supported evaluation at SPH was designed as quality improvement trial: get the device onto the floor, let nurses use it with patients, observe the response, and collect direct feedback from the clinical team.
What Dr. Flexman and her research team observed was striking in its speed and organic enthusiasm. Patients took to the platform more quickly than most new interventions. Some loved it, requesting it for as long as possible. Nurses reported that it was able to occupy patients during vulnerable periods, keeping them calmer and giving nursing staff the space to complete their work uninterrupted.
Then something unexpected happened. The trial was so successful that nurses began using the device on patients outside the study protocol.
“Now we’re in a second phase where we’ve started our clinical study,” says Dr. Flexman, “And we’re having to shut people down from using it on other patients because the nurses want to use it more broadly. We can’t do that until the trial is done. But it’s a testament to the fact that they’ve found real benefit for patients.”
The evaluation phase also generated invaluable product feedback: the need for clearer privacy labelling on the camera, the inadequacy of built-in speakers in noisy ICU environments, and opportunities to expand the platform’s content library. These findings are now directly shaping MindfulGarden’s V.2 development.
From Evaluation to Evidence
With the PHC Anesthesiology evaluation complete, the partnership has now seeded a fully powered randomized pilot trial at St. Paul’s Hospital funded by the Canadian Anesthesiologists’ Society.
The trial is designed to go beyond the question of whether MindfulGarden works, to answer how and for whom. Is it reducing anxiety? Preventing the onset of delirium? Reducing medication administration? Understanding the mechanism of action is essential for scaling the intervention across different patient populations and hospital settings.
MindfulGarden is providing the devices for the trial — a contribution that Dr. Flexman notes was critical to making it possible. The relationship between innovator and clinical investigator has become symbiotic: the researchers get access to a promising tool and real-world data; MindfulGarden gets the independent evidence it needs to move into broader adoption and guidance to procurement pathways.
“Everything we do has to be informed by clinicians. We need clinical evidence, user evidence, and we need to know where it can be made better. There’s no way to unlock that, without partners like PHC Ventures and St. Paul’s Hospital.”
— Mark Ross, Co-Founder & CTO, MindfulGarden
What This Partnership Proves
MindfulGarden’s journey with PHC Ventures offers a compelling model for how health technology innovation should work. A clinically grounded idea, a rigorous real-world evaluation, a clinical champion with genuine shared interest, and an institutional partner with the infrastructure and credibility to make it all happen inside a health system.
For other health tech startups navigating the same path, Mark Ross is direct in his advice: “Find the right champion first. Get your device into the hands of end users as soon as possible. Do not design and develop without talking to your users. And then bring the clinical side and the business operations side together with a shared north star. What are we trying to do for patients, and what does that mean for operations?”
PHC Ventures is now guiding MindfulGarden through the commercialization pathway, helping translate clinical proof into sustainable adoption across Canadian hospitals, and potentially far beyond.
Delirium has been called “the epidemic within the pandemic,” a condition that is globally ubiquitous, enormously costly, and largely unaddressed. MindfulGarden is working to change that, one calming interaction at a time.