Innovative Technology Developed and Distributed by PHC-lead Team Empowers Rural Physicians
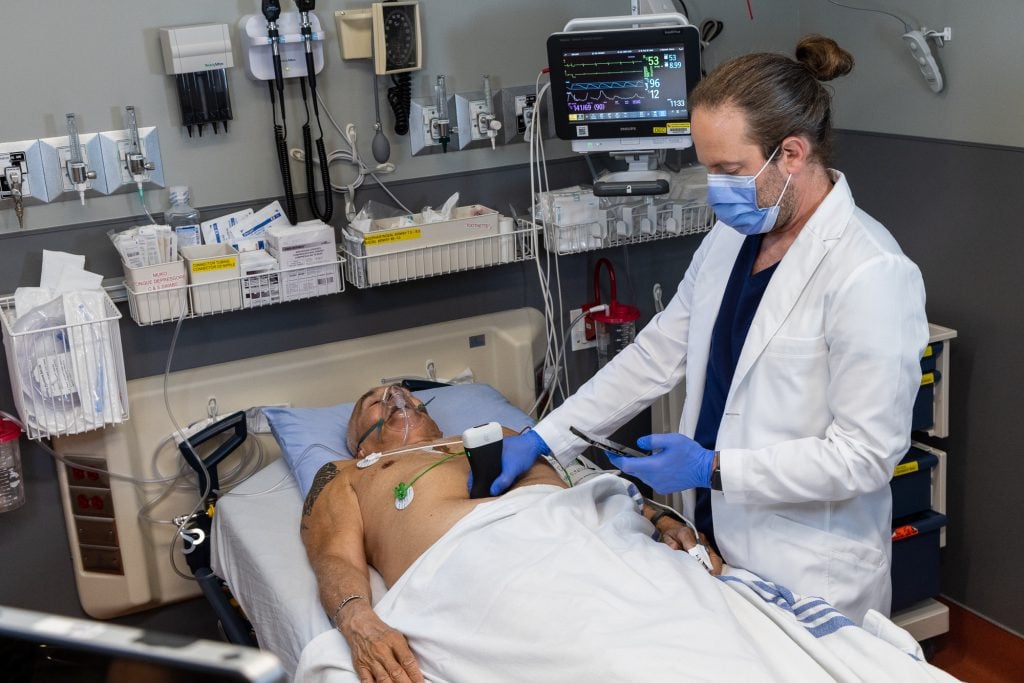
Ultrasounds are key clinical tools used to diagnose many conditions, but access to traditional ultrasound scans is limited by machine availability and the ability analyze the results. Patients, particularly those in in rural or remote communities, can face long wait times or need to travel long distances to access these scans.
Providence Health Care is a member of DIGITAL, formerly Canada’s Digital Technology Supercluster, which aims to fast track Canadian digital technologies than improve health and wellbeing, protect our environment, and drive economic productivity. In collaboration with PHC Ventures, Change Healthcare, Clarius Mobile Health, the University of British Columbia and the Rural Coordination Centre of BC, with support from St. Paul’s Foundation, DIGITAL’s Intelligent Network for Point-of-Care Ultrasound (IN-PoCUS) project developed, distributed and studied the impact of handheld ultrasounds.
These devices combine machine learning and a cloud-based platform to create a point-of-care ultrasound network to deliver faster, more accurate diagnoses and empower clinicians to make more informed decisions. By being able to distinguish between smaller issues and emergencies, this technology can help streamline care and potentially save lives.
Flexible technology can help reduce delays
“One of the powers of the ultrasound technology is that it can be used on virtually any organ system,” says Dr. Oron Frenkel, an Advancing Health scientist and St. Paul’s Hospital emergency physician who was the clinical lead on this supercluster project. With handheld ultrasounds, physicians can scan multiple parts of the body with one device, instead of having to go through a longer process of scanning a particular area with traditional imaging. This can help reduce common delays.
Dr. Frenkel is no stranger to portable ultrasound technology. He completed a fellowship training in point-of-care ultrasound use at Alameda County Medical Centre in Oakland, California, and for several years ran his own point-of-care ultrasound education program through Providence Health Care, training emergency physicians from across BC, including those from rural areas.
During the DIGITAL project, Dr. Frenkel was able to use the contacts he made through this training to connect with the Rural Care Coordination Centre of BC, who became a critical partner.
Research shows benefits to rural doctors
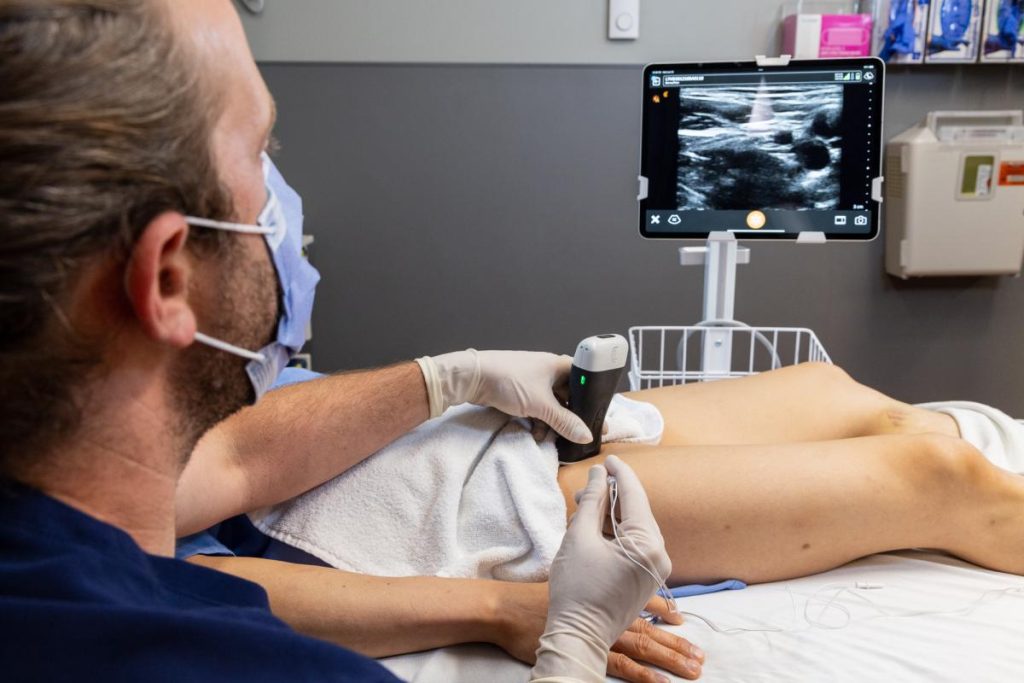
IN-PoCUS supports doctors with AI technology integrated into the device that provides visual feedback and reduces the need for specialized training, as well as a robust educational network that gives them access to guidance from specialists when needed. The project distributed over eighty handheld ultrasound devices to rural doctors in British Columbia.
A qualitative study of this program, co-authored by Dr. Frenkel, examined the perspectives of rural family physicians on IN-PoCUS and its impact on the care they provide. It found that IN-PoCUS empowered physicians to make better decisions, and those physicians felt that they had more tools at their disposal to provide better care. The handheld ultrasounds were able to provide them with valuable real-time feedback, which was especially significant in communities without access to formal ultrasound services. IN-PoCUS users even reported an increase in job satisfaction.
“The qualitative research piece really highlighted how impactful having access to this diagnostic technology is for rural physicians,” says Dr. Frenkel.
A quantitative study looking into the quality of family doctor’s image interpretation versus that of specialists is still in progress. It will help identify areas where better support could be provided.
New tool predicted to become standard of care
While IN-PoCUS is not a replacement for traditional scans and specialists, it is a valuable addition to doctors’ toolboxes. Dr. Frenkel believes it is only a matter of time before handheld point-of-care ultrasounds become part of the standard of care.
Any new technology requires a certain amount of training and education to learn to use safely and effectively. As handheld point-of-care ultrasounds become more prevalent in the medical training environment, and more doctors come into the field who have trained with it as part of their education, it will be seamlessly integrated into their clinical practice.
“I would predict, in the next ten years, it will be quite widespread. Our goal, ultimately, is that every doctor will have one in their hand,” says Dr. Frenkel.
You can watch a video spotlighting the project here.